Ureteral stent: lifestyle and behavioral advice
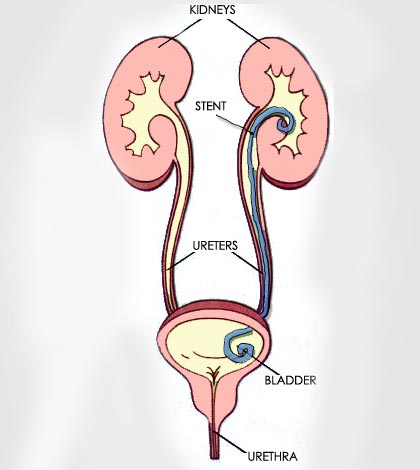
A ureteral stent is a small tube inserted between the kidney and the bladder to facilitate urine flow in the presence of obstruction, stones, or after a urological procedure. Its presence may cause discomfort such as burning, frequent urination, or mild flank pain, but with some daily precautions, it is possible to reduce symptoms and maintain a good quality of life.
This article provides practical guidance on how to manage a ureteral stent best: from proper hydration to allowed physical activity, as well as behaviors to avoid and warning signs that require medical attention. The information is purely educational and does not replace specialist advice, but it can help patients live more comfortably during the period the stent remains in place.
Discomfort related to ureteral stent placement is generally divided into three phases:
1. Acute Phase (First 2–3 days)
This is the most uncomfortable period. The bladder and ureter react to the presence of a foreign body with intense spasms. During this phase, it is common to experience:
- Strong urinary urgency and frequency
- Flank pain during urination (reflux-related pain)
- Presence of blood in the urine (hematuria), especially with movement
2. Adaptation Phase (From day 4 until removal)
After the first few days, the body tends to "adapt." Symptoms do not disappear completely but become milder and more tolerable. Many patients report that discomfort reappears mainly after physical exertion or long walks.
3. Post-Removal Resolution
The good news is that symptoms usually disappear almost immediately (typically within 24–48 hours) after stent removal. Once the tube is removed, bladder irritation subsides and the ureter returns to normal function.
Practical Advice
Hydration:
Drink plenty of water (about 2 liters per day). This helps "flush" the bladder, reducing irritation caused by small blood clots and preventing encrustation on the stent.
Physical Activity:
Avoid intense physical effort or sudden movements, as the stent is "free" within the bladder and movement may cause micro-trauma to the mucosa, increasing hematuria.
Urination:
Avoid holding urine for too long, as this increases backward pressure toward the kidney, leading to the typical flank pain during urination.
Medications (only under medical prescription)
Medications are the mainstay for relaxing the ureteral and bladder muscles and improving symptom tolerance:
- Alpha-blockers (e.g., Tamsulosin, Silodosin): First-line treatment. They reduce ureteral pressure and bladder spasms, significantly improving pain and urinary symptoms.
- Antimuscarinics (e.g., Solifenacin, Oxybutynin): Used to reduce urgency and frequency by acting on involuntary bladder contractions caused by stent irritation.
- Combination therapy: Often, combining an alpha-blocker with an antimuscarinic provides the best results.
Pain Management
- NSAIDs (e.g., Ibuprofen, Ketoprofen): Highly effective for flank pain and local inflammation.
- Paracetamol (Acetaminophen): Can be used as an alternative or in combination, although it is less effective on the inflammatory component.
When to Seek Medical Attention
While mild burning and pinkish urine are normal, you should go to the Emergency Department if you experience:
- Fever (possible sign of infection)
- Persistent bright red blood with clots that make urination difficult
- Severe pain that does not respond to prescribed medications